ON THIS PAGE: You will find some basic information about this disease and the parts of the body it may affect. This is the first page of Cancer.Net’s Guide to Neuroendocrine Tumor of the Pancreas. Use the menu to see other pages. Think of that menu as a roadmap for this entire guide.
About neuroendocrine tumors
A tumor begins when the DNA of healthy cells is damaged, causing the cells to change and grow out of control, forming a mass. A tumor can be cancerous or benign. A cancerous tumor is malignant, meaning it can grow and spread to other parts of the body if it is not found early and treated. A benign tumor means the tumor can grow but will not spread. A benign tumor usually can be removed without it causing much harm.
A neuroendocrine tumor (NET) begins in the specialized cells of the body’s neuroendocrine system. These cells have traits of both hormone-producing endocrine cells and nerve cells. They are found throughout the body’s organs and help control many of the body’s functions. Hormones are chemical substances that are carried through the bloodstream to have a specific effect on the activity of other organs or cells in the body. All NETs have the potential to become metastatic. Most NETs take years to develop and grow slowly. However, some NETs can be fast-growing. See the Stages and Grades section to learn more.
NETs can begin in any part of the body, including the pancreas. Pancreas NETs may also be called pancreatic NETs. This type of tumor used to be called an islet cell tumor. NETs are more commonly found in the gastrointestinal (GI) tract (learn more about NETs of the GI tract) or in the lungs (learn more about NETs of the lung). GI tract NETs and lung NETs are sometimes also called carcinoid tumors. Rare types of NETs that develop in or on an adrenal gland are called pheochromocytoma or paraganglioma. Learn more about NETs that develop in other parts of the body.
About pancreas NETs
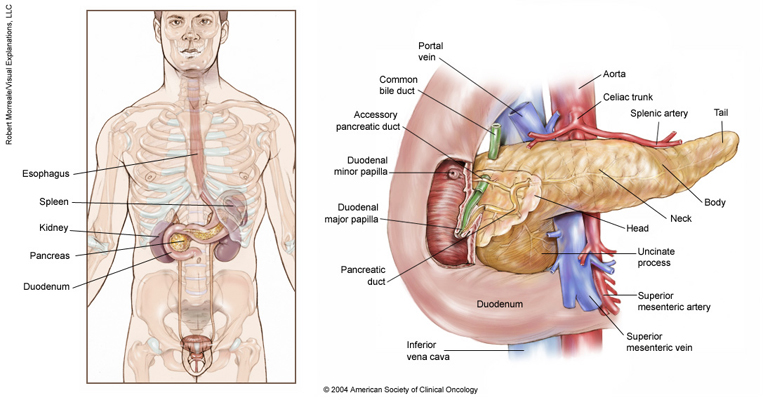
Approximately 7% of NETs develop in the pancreas. The pancreas is a pear-shaped gland located in the abdomen between the stomach and the spine. It is about 6 inches long and is made up of 2 major components:
-
Endocrine component. This part of the pancreas is made up of specialized cells clustered together in islands within the organ, called islets of Langerhans. These cells make hormones, specifically insulin. Insulin is the substance that helps control the amount of sugar in the blood. Pancreas NETs develop in the islets of Langerhans in the endocrine component.
-
Exocrine component. This component is made up of ducts with small sacs called acini at the end. It produces specialized proteins called enzymes that are released into the small intestine to help the body digest and break down food, particularly fats.
A pancreas NET is very different from pancreas adenocarcinoma, which is a more common type of pancreatic tumor. Adenocarcinoma of the pancreas begins in the exocrine component. You can read about that type of pancreatic cancer in another section of this website.
Subtypes of pancreas NETs
A pancreas NET may be classified as either “functional” or “non-functional.” The cells in a functional pancreas NET make and release measurable amounts of hormones and other substances that cause symptoms. A non-functional pancreas NET either does not release substances or does not release enough substances to cause symptoms. Most pancreas NETs are non-functional. Because of a lack of symptoms, these tumors are usually diagnosed at a more advanced stage.
There are 5 major classifications of functional pancreas NETs. These types are based on the hormone that the cells normally make. Some tumors can make 1 or more of these hormones at the same time.
-
Insulinoma. This type of tumor makes too much insulin, causing hypoglycemia, also known as low blood sugar. An insulinoma is more likely to be noncancerous. About 10% become cancerous.
-
Gastrinoma. A gastrinoma is a pancreas NET that makes too much gastrin, a hormone that causes acid production in the stomach. Too much stomach acid can cause severe ulcers, a condition called Zollinger-Ellison syndrome.
-
Glucagonoma. A glucagonoma is a pancreas NET that makes too much of the hormone glucagon. Unlike an insulinoma, a glucagonoma causes hyperglycemia, a condition where there is too much sugar in the blood.
-
VIPoma. A VIPoma starts in the cells in the pancreas that make vasoactive intestinal peptide (VIP), a hormone that helps move water into the intestines. Too much VIP can cause chronic, watery diarrhea, which causes a condition called Verner-Morrison syndrome.
-
Somatostatinoma. A somatostatinoma usually develops in the head of the pancreas. A somatostatinoma may make a hormone called somatostatin. This hormone stops the production of several other hormones, such as growth hormone, insulin, and gastrin.
Looking for More of an Introduction?
If you would like more of an introduction, explore these related items. Please note that these links will take you to other sections on Cancer.Net:
-
Find a Doctor. Search for a specialist in your local area using this free database of doctors from the American Society of Clinical Oncology (ASCO).
-
Medical Terms. Learn what common medical phrases and terms mean.
The next section in this guide is Statistics. It helps explain the number of people who are diagnosed with a pancreas NET and general survival rates. Use the menu to choose a different section to read in this guide.