ON THIS PAGE: You will find some basic information about this disease and the parts of the body it may affect. This is the first page of Cancer.Net’s Guide to Melanoma. Use the menu to see other pages. Think of that menu as a roadmap for this entire guide.
About the skin
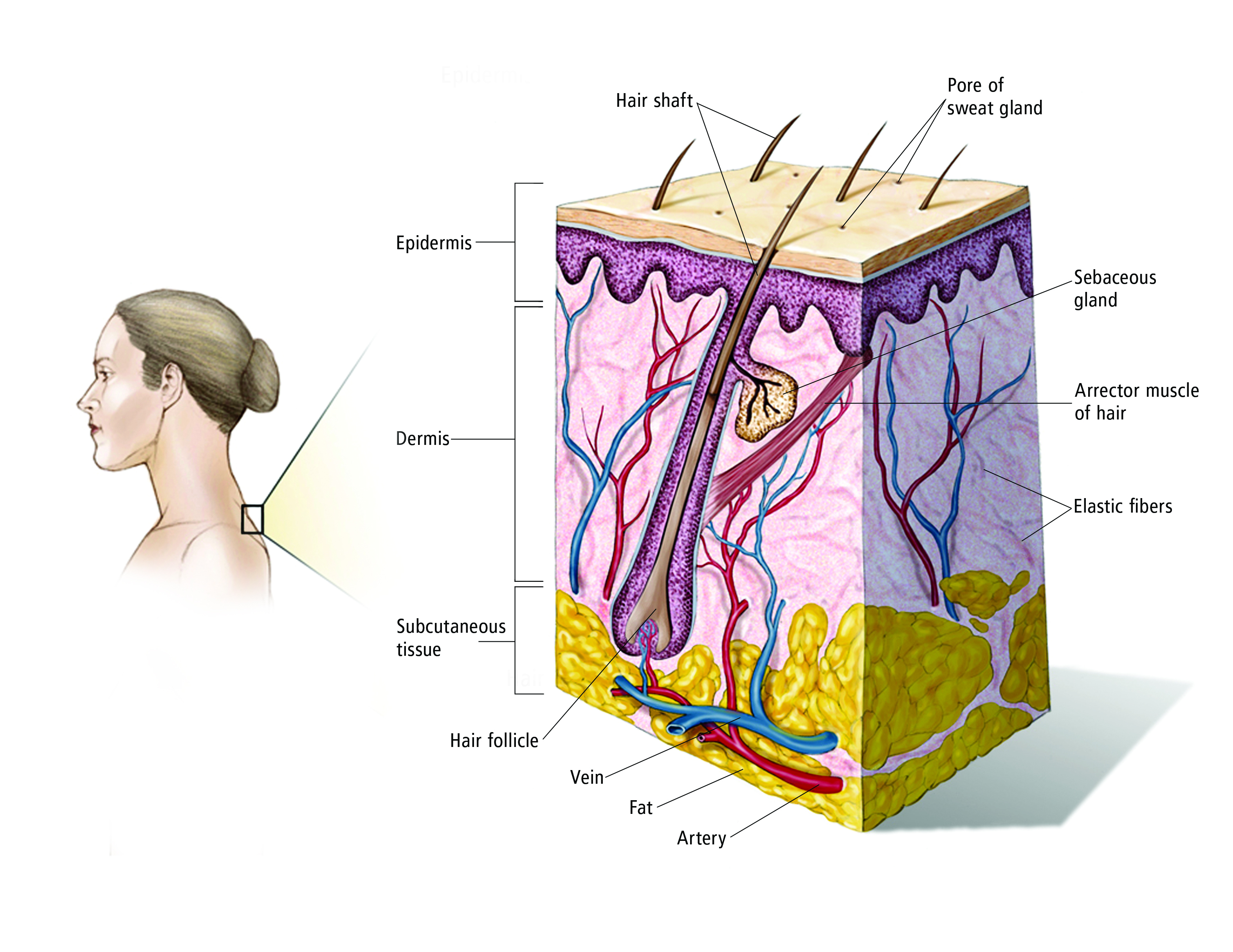
The skin is the largest organ in the body. It protects against infection and injury and helps regulate body temperature. The skin also stores water and fat and produces vitamin D.
The skin is made up of 3 main layers:
-
Epidermis: The outer layer of skin.
-
Dermis: The inner layer of skin.
-
Hypodermis: The deep layer of fat.
About melanoma
The deepest layer of the epidermis, located just above the dermis, contains cells called melanocytes. Melanocytes produce the skin’s pigment or color.
Melanoma begins when healthy melanocytes change and grow out of control, forming a cancerous tumor. A cancerous tumor is malignant, meaning it can grow and spread to other parts of the body. Sometimes, melanoma develops from a normal mole that a person already has on their skin. When this happens, the mole will undergo changes that usually can be seen, such as changes in shape, size, color, or the border of the mole (see also Symptoms and Signs). Other times, melanoma may develop on skin where there is no existing mole.
Melanoma can develop anywhere on the body, including the head and neck, the skin under the fingernails, the genitals, and even the soles of the feet or palms of the hands. Melanoma may not be colored like a mole. It may have no color or be slightly red, which is called amelanotic melanoma.
When found early, melanoma can often be cured with surgery. However, melanoma is one of the most serious forms of skin cancer. It can grow deep into the skin; this is called invasive melanoma. It can also invade blood vessels and spread to lymph nodes and distant parts of the body; this is called metastatic melanoma.
This section focuses on cutaneous melanoma, which is melanoma that first develops in the skin. Less commonly, melanoma can develop in the mucous membranes that line the mouth, the gastrointestinal tract, the vagina, and other locations around the body. This type of melanoma is called mucosal melanoma. Uveal melanoma is melanoma that develops in the eye.
For information about other types of skin cancer, visit the section on non-melanoma skin cancers.
Looking for More of an Introduction?
If you would like more of an introduction, explore this related item. Please note that these links will take you to other sections on Cancer.Net:
-
ASCO Answers Fact Sheet: Read a 1-page fact sheet that offers an introduction to melanoma. This free fact sheet is available as a PDF, so it is easy to print.
-
Cancer.Net En Español: Read about melanoma in Spanish. Infórmase sobre melanoma en español.
-
Find a Cancer Doctor. Search for a cancer specialist in your local area using this free database of doctors from the American Society of Clinical Oncology (ASCO).
-
Cancer Terms. Learn what medical phrases and terms used in cancer care and treatment mean.
The next section in this guide is Statistics. It helps explain the number of people who are diagnosed with melanoma and general survival rates. Use the menu to choose a different section to read in this guide.